A new study posted on MedrXiv sheds light on the potential of breath analysis as a powerful, non-invasive diagnostic tool for Trimethylaminuria (TMAU) and TMAU-like conditions. One of the most interesting observations is the detection of Propylene Oxide in exhaled breath suggesting its delayed elimination and offering a promising marker for misunderstood and underdiagnosed conditions.
TMAU-like (yet negative to choline-challenge-based test) and "People Are Allergic To Me" (PATM) conditions, characterized by the emission of odorous or irritating Volatile Organic Compounds (VOCs), have long challenged the medical community due to the lack of non-challenge-based diagnostic procedures.Using advanced gas chromatography-mass spectrometry, researchers analyzed the breath of 23 individuals exhibiting TMAU-like symptoms. They discovered that Propylene Oxide, alongside other VOCs, some of which were previously associated with PATM, can effectively discriminate between individuals who have tested positive for TMAU at some point and those who have not. This method demonstrated impressive accuracy, precision, and recall rates, making it a potential cornerstone for future diagnostic strategies.
Propylene Oxide's presence in breath samples particularly stood out in the study. This compound was more abundant in individuals that never tested positive for TMAU, potentially pointing to unique metabolic processes or environmental interactions that could be pivotal in understanding and managing TMAU-like conditions.
Propylene Oxide (PO) is a prevalent chemical found not only on Earth, owing to its widespread use in industrial and consumer applications, but also in the Milky Way. It leaves more significant marks on the human body than previously thought. Mass production contributes to its omnipresence, and exposure can occur through various sources such as cellulose acetate film, wood shavings, and paper cups. Despite efforts to eliminate gas residues, accidental exposure still occurs, particularly among workers involved in sterilization processes. Additionally, foods treated with PO as a fumigant may contain residues of the chemical.
PO has been detected in human breath following exposure to Propylene (PE), a combustion product found in forest fires, cigarette smoke, and vehicle exhaust. Indoor exposure is typically higher than outdoors due to residential activities like cooking, and urban areas tend to have higher concentrations than rural regions. Workers in specific industries may face elevated exposure levels, such as firefighters and refinery plant operators. PEG in cosmetic products can also be contaminated with propylene oxide. Furthermore, Propylene Glycol (PG) in cigarettes and e-liquids can be converted to PO, contributing to exposure.
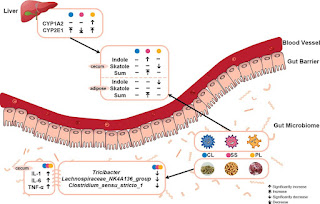
Other compounds mentioned in the paper were markers of oxidative stress Hydroperoxide, hexyl; Hexanal; Decane, 2-methyl-; Tetradecane; Decane, 2,6,6-trimethyl- and D-limonene. 2,2,3-trimethylnonane was one of compounds associated with breath odor.
This research emphasizes the need for personalized diagnostic approaches, considering the significant variability in VOCs among individuals. Such tailored strategies could lead to more accurate diagnoses and better management of conditions that currently lack specific treatments.