Functional medicine provides a powerful model known as the 5R Approach (Kim, 2024), which builds on the original 4R framework (Remove, Replace, Reinoculate, and Repair; Liška, 2003)) by adding a crucial final step: Rebalance.
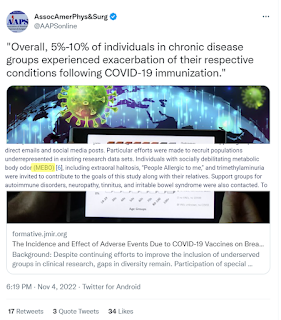
This method is particularly valuable in treating gut dysbiosis, a condition in which the ratio of beneficial and harmful bacteria in the intestine is disrupted, leading to inflammation, poor digestion, and systemic health issues. Research has linked gut dysfunction to chronic conditions such as rheumatoid arthritis, eczema, and neurological disorders (Liška, 2003) as well as nonsyndromic body odor (Gabashvili, 2020)
1. Remove: Eliminating Triggers of Gut Dysfunction
The first step in healing the gut is removing harmful elements that contribute to dysbiosis and inflammation. These include:
Pathogens – Overgrowth of harmful bacteria, yeast (Candida), or parasites.
Inflammatory Foods – Processed sugars, refined carbohydrates, artificial additives, and common allergens (gluten, dairy, soy).
Toxins & Medications – Overuse of antibiotics, NSAIDs, and environmental toxins disrupt gut flora and damage the mucosal lining.
📌 An elimination diet can help identify specific food triggers. GI map test as well as testing for known gut infections (such as H.pylori, HSV, CMV, giardia or Candida spp.) can also guide targeted interventions.
2. Replace: Supporting Digestive Function
Once harmful elements are removed, the next step is to restore digestive efficiency by supplying essential compounds for proper digestion:
Digestive Enzymes – Help break down food and enhance nutrient absorption.
Stomach Acid (HCl) – Supports protein digestion and prevents bacterial overgrowth.
Bile Salts – Assist in fat digestion and absorption, especially if gallbladder function is compromised.
📌 Consider incorporating enzyme-rich foods like papaya (papain) and pineapple (bromelain) or taking targeted supplements.
3. Reinoculate: Restoring Beneficial Bacteria
A diverse microbiome is essential for digestion, immunity, and gut-brain interactions. Research suggests that early-life gut health, influenced by factors like breastfeeding, can impact long-term microbial balance (Ley et al., 2021).
📌 Aim for a variety of fiber-rich foods, prebiotics (asparagus, bananas, onions) and probiotic-rich fermented foods to support microbiome diversity, rather than relying solely on probiotic supplements.
4. Repair: Healing the Gut Lining
An increase in harmful bacteria can damage the intestinal mucosal cells, contributing to leaky gut syndrome and systemic inflammation (Kim, 2024). Repairing the gut lining is crucial for long-term resilience.
Key nutrients that aid gut repair include:
L-glutamine – An amino acid essential for intestinal wall regeneration.
Collagen & Bone Broth – Provide glycine and proline, which strengthen the gut barrier.
Zinc & Vitamin A – Promote mucosal healing and immune function.
Omega-3 Fatty Acids – Reduce inflammation and support tissue repair.
5. Rebalance: Addressing Lifestyle Factors
The final and often overlooked step in gut healing is rebalance—restoring the mind-body connection and lifestyle habits that influence digestive health. The gut-brain axis plays a crucial role in regulating digestion, with parasympathetic “Rest and Digest” responses supporting motility and secretions (Gantzer, 2021).
To rebalance:
Stress Management – Chronic stress disrupts gut function and increases inflammation. Practices like meditation, deep breathing, and yoga enhance parasympathetic regulation.
Sleep Quality – Poor sleep affects gut motility and microbiome balance. Aim for 7-9 hours of uninterrupted sleep.
Physical Activity – Moderate exercise supports gut health by improving motility and microbiome diversity.
📌 Engage in mindful eating—slow down, chew thoroughly, and avoid distractions to support optimal digestion.
The 5R Approach offers a structured, evidence-based method for restoring gut health and preventing chronic disease. Whether dealing with digestive disorders, autoimmunity, or general well-being, this framework provides a sustainable path to healing.
By removing harmful triggers, replacing digestive supports, reinoculating the microbiome, repairing the gut lining, and rebalancing lifestyle factors, we can achieve long-term gut resilience and overall health.
REFERENCES
Gabashvili IS Cutaneous Bacteria in the Gut Microbiome as Biomarkers of Systemic Malodor and People Are Allergic to Me (PATM) Conditions: Insights From a Virtually Conducted Clinical Trial JMIR Dermatol 2020;3(1):e10508 doi: 10.2196/10508
김규남. 기능의학적 5R 치료의 근거와 적용. Journal of Korean Institute for Functional Medicine. 2024 May;7(1):1-8: Kyu-Nam Kim Korean Society of Functional Medicine Journal of Korean Institute for Functional Medicine Vol.7 No. 1 2024.05 1 - 8 (8 pages) DOI : 10.32581/jkifm.2024.7.1.1
Liska DJ, Lukaczer D. Gut dysfunction and chronic disease: the benefits of applying the 4R GI restoration program. ANSR-Appl Nutr Sci Rep. 2003:1-8.
J. Gantzer Acta Supporting Gut Health by Homeostasis and Intrinsic Mechanisms. Scientific Neurology 1 November 2021 https://www.actascientific.com/ASNE/pdf/ASNE-04-0444.pdf